|
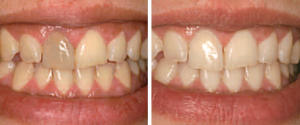
One of the causes of tooth discoloration is receiving root canal treatment. For one reason or another a front tooth might undergo such treatment. The tooth after this becomes “dead”. meaning there is no nerve and no blood supply in the core of the tooth. If the tooth required such treatment due to trauma, sometime blood pigmentation makes the discoloration worse. What can be done? usually a traumatized toth requires a porcelain crown. However if the tooth structure was not damaged significantly. A porcelain crown might be avoided, and to restore the white color fo the tooth, we can do Internal bleaching. What does that involve? – after finishing the root canal. we end up with a space where it was occupied by the nerve, this space is called pulp chamber. we drill about 1-2mm into the root canal from the chamber. – A bleaching medicament is placed into the chamber and sealed. – following the manufacturer’s instructions, we leave this medicament within the tooth for a certain period of time. then it might be reapplied. – when the treatment is finished, the medicament is removed and a definite filling is used to close the access cavity. so in essence in this procedure, we are whitening the tooth from inside out. So it is called internal bleaching. sometimes even if the tooth is going to be restored with a porcelain crown, such procedure is advised because if the tooth is too dark, it might affect the resulting shade of the porcelain giving us an undesirable shade. How good is it? It is quite effective in bleaching a tooth, however sometimes it might be combined with an external option. The darker the tooth is, then less chance for the treatment to work by itself. But for the most common cases, it is quite effective and no more whitening is required. Conclusion:If you had a trauma and your tooth appears darker, the solution might not be as costly as you think. talk to us to see if you can have internal bleaching.
0 Comments
Tooth decay is the most common disease entity for adults and children alike. You need to understand the process of tooth decay to prevent it. Prevention is better than cure. Toot decay is preventable. For tooth decay to happen, you need four elements: 1- Toot structure; if you have porcelain, or dentures, they will not get decayed, but remember that there is a tooth under that porcelain that can indeed get decay. 2- Sugar material, this is what gets transformed into acid by the next element: 3- bacteria. you cannot eliminate bacteria from your mouth, they colonize our moths via food and air. they form a layer called dental plaque and use the sugar to produce acid 4- Time; the bacteria need time to digest the sugar and produce acid. then time is needed for the acid to break down your tooth. once the tooth starts to desolve under the effect of acid, it gets weaker and starts to break down forming a hole “cavity” in your tooth so prevention starts with breaking the cycle. How to work on these elements to prevent tooth decay:1- tooth structure: a- first try to make this tooth less exposed to food, so try not to snack between meals b- try to keep your tooth, plaque-free by brushing after meals and flossing. c- use Xylitol gum, this substance prevents the bacteria from adhering to your tooth structure. d- don’t miss your routine check and clean, keeping your tooth surface smooth free of calculus means less chance for germs to adhere to it. e- keep checking old fillings and crowns. if the dentist sees a rough margin of a filling, better fix it. f- make sure to clean the margins of crowns. these are rough surfaces and bacteria adhere to them easily. g- ask us to place fissure sealants on your teeth. to prevent bacteria from colonizing these fissures that are out of reach, even for your tooth brush. h- make sure to use fluoridated tooth paste, that strengthens your tooth structure, and also don’t miss your 6 monthly fluoride application. 2- Sugar material a- always go for the sugar-free option. b- avoid snacking between meals c- after each meal, brush your teeth, to get rid of residual sugar. d- Sugar-less gum. this encourages salivation, which washes your teeth. use Xylitol gum, Xylitol has also been shown to help remineralize our teeth’s enamel 3- Bacteria: a- brush at least twice a day for two minutes each time. to get rid of dental plaque b- floss once a day to remove the bacteria between teeth c- use anti-bacterial mouth wash.These oral rinses are designed to decrease cavity causing bacteria in the mouth while utilizing fluoride to strengthen enamel against breakdown. If brushing and flossing is done properly, use of an oral rinse should complete the protection against tooth decay Other preventive measures:– For snacks: best snacks for your dental health include raw vegetables, fruits, and nut. Apples are the perfect snack for dental health as they act as a tooth cleaner and whitener. They are able to clean your teeth by the abrasive action of the skin and hard inner surface of the apple, they have malic acid which helps remove surface stain and keep teeth whiter. So next time you are looking for a midday snack pick up an apple. – Fluoridated water This very important for children. However use water that has been fluoridated by the local council, as excessive fluoride can be harmful to your teeth. Conclusion:Tooth decay is preventable juts by following simple rules and keeping in mind that your teeth can suffer from what you do and what you eat. Make sure to keep your dental visits. Maybe one day, we will have a generation free of tooth decay . Until then, we need to follow the steps above to maintain good oral health.
We might lose a tooth or more in many ways like trauma, gum disease, fracturing in heavily filled teeth or after root canal therapy, infection, and decay. One of the options to replace missing tooth or teeth is by having dental implants.. Dental Implants give the dentist and patient a better way to restore that smile and return it to its youthful appearance. What Are Implants? The main part of a dental implant is called a fixture and replaces the root of the tooth. It is placed into the jaw bone like an infrastructure to support what will come afterwards above it. The success rate for implants surpasses 90% This infrastructure can support a single tooth or they can be planned to support more, whether with a removable denture or fixed bridge. The cosmetic benefits of implants are obvious as they preserve the bone, gums and teeth. Restoring the natural smile. Best Options For Dental Implants Dental implants are planned on individual basis, as their placement depends on many factors that cannot be generalized, like bone availability, bone quality, condition of remaining teeth, and medical condition. –For A Single Tooth. This can be a straight forward procedure. It might involve some bone grafting firt or together with implant placement. The fixture supports another part called abutment that is screwed to the fixture and protrudes through the gums. Then a crown is fabricated to either get screwed or cemented to the abutment. This will restore the tooth and preserve bone, it will also give the gums its natural appearance and contours around the crown. Bridges are another option of replacing a missing tooth, but that will involve trimming sound tooth structure of the adjacent teeth, which might cause nerve damage to the these teeth, warranting their ultimate loss. –For Multiple Teeth. when more than one tooth is missing, either one implant is used per tooth, or implants can be sued to hold a bridge. Or implants can be sued to hold a removable denture. –For All Teeth. Implants can be used to give us more comfortable dentures by securing them with two implants that hold a denture. Or implants can be used to hold the entire dentition which is fixed by screws and can be removed by the dentist only. New techniques involve using only 4 implants to support an entire dentition. Dental Implants ConclusionImplants are the better option or replacing missing teeth. They are not the only option, but they definitely the closest thing to natural teeth, in function and cosmetics.please tell us if you had an experience with implants or you would like to share your opinion.
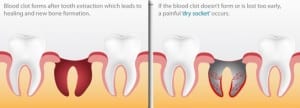
Dry socket (also called alveolar osteitis) is an extremely painful dental condition that can occur after removal (extraction) of a permanent adult tooth. Having a tooth removed is generally not something anyone looks forward to. Most people understand there will be some level of discomfort following the procedure. Many are given a prescription for pain medication before leaving their dentist. Most people in fact do not even need to get the prescription filled. However, when a patient experiences what is called a dry socket the pain can become quite intense and linger for days. Very few people are affected by dry socket. The development of Dry socket after a tooth extraction occurs in only about 2-3% of patients. For those who experience dry socket it can be a very scary experience. Fortunately dry socket is treatable. A dry socket occurs when the blood clot at the site of the tooth extraction has never fully formed, has broken free, or has dissolved before the wound has had a chance to fully heal. The blood clot is the protective layer for the underlying bone and nerves, it begins the process of healing so that gum tissue and bone can refill the area. When the clot is gone the bone and nerves are now exposed to the outside air, food, fluid, and anything else that enters the mouth. This can lead to a dry socket with sharp, aching pain that can last for 5-6 days, and in the case of a patient taking fosamax type drugs the pain can last for weeks. A dry socket is considered the most common complication following tooth extractions. It happens more frequently with extraction of impacted wisdom teeth, in patients with poor blood flow to the socket, (smokers, patients taking fosamax), delayed healing (diabetics ). The pain begins to build and develop about 2-4 days following the procedure. Signs and Symptoms of Dry SocketSigns and symptoms of dry socket may include: -Sharp, aching pain within 2-4 days after a tooth removal. -Partial or total loss of the blood clot at the tooth extraction site. You would be able to visually notice a deep hole or space where tooth used to be, that weeps fluid when pressed vs a blood clot overlaying the site. -Bone that is visible upon visual examination in the socket -Pain that radiates from the socket to your ear, eye, temple or neck on the same side of your face as the extraction -Abnormally bad breath or a foul odour emanating from your mouth. This will coincide with having a bad taste in your mouth as well. -If you have swollen lymph nodes around your jaw or neck, this is a sign of infection and you need to be seen by your dentist immediately. Over the counter medications by themselves will not control the symptoms. We will need to begin treatments to lessen pain and allow for healing to take place. Treatment of Dry SocketTaking a nonsteroidal anti inflammatory drug (like ibuprofen) can help to ease the pain but probably will not be enough to take it away completely. When the pain persists you should call us immediately. We may prescribe you a stronger pain medication to allow the pain to subside for you or give you anesthesia in the office to relieve some of the symptoms for a little while anyway. Paste for Dry Socket What will we need to do for the dry socket? we will need to numb and clean the tooth socket. This will allow for removal of any debris from the space where the tooth once was, and allow for rebleeding into the site. We may then fill the socket with a medicated dressing or a special paste to promote healing and soothe the symptoms. The dressing may need to be reapplied if pain persists after three days. Warm cloth on the outside of the face also helps promote blood flow. An antibiotic may also be prescribed at this point to prevent an infection from forming. At home care will include rinsing with salt water and being careful what you eat and how you eat it, ( avoiding the side where the dry socket is ). The site will usually heal completely following treatment in 1-2 weeks. Who is most likely to get a Dry Socket?Some patients will be more likely than others to get a dry socket after a tooth extraction. These include the following:
–Smokers. Patients who smoke have twice the chance of developing dry socket over those who do not. smoking also is believed to slow the healing process. –Poor oral hygiene. Those with poor oral hygiene will have an increased risk due to the amount of bacteria in the mouth. Will be difficult to maintain a sterile field when removing tooth. –Having wisdom teeth (3rd molars) extracted. Increased trauma to area during procedure is one of the indicators for increasing the possibility for the development of dry socket. 3rd molars tend to be more difficult to remove especially if they are fully or partially impacted. –Previous history of dry socket. If you have had dry socket previously, you are more likely to develop it after another extraction. –Use of birth control pills. Contraceptives which contain estrogen effect the blood clotting system of the body. So we see an increased incidence in dry socket in patients on oral contraceptives. Rinsing and spitting a lot or smoking after having a tooth extracted also can increase your risk of getting dry socket. These activities will increase chances of the blood clot becoming dislodged. Following the removal of a tooth, it is very important to follow all instructions given to you. If you are unsure of anything you must ask or call back. At first sign of pain or discomfort call your dentist to be sure it is not something more serious. As always, maintain a regular schedule visiting your dentist, as well as keeping an open communication with your dentist. This will make you feel comfortable asking questions and knowing you are getting the proper information to care for your oral health. |
AuthorArticles are written by Dr M Hajarat. Archives
July 2024
|
|
Niagara Park Dental
3 / 16 Washington Avenue Niagara Park, NSW 2250 Email: [email protected] Phone: (02) 4329 3003 |
HOURS
Mon 9:00 - 5:30 Tue 9:00 - 5:30 Wed 9:00 - 5:30 Thu 9:00 - 5:30 Fri 9:00 - 5:30 |
|